Case based-review
Non-healing wounds – the choice of surgery when conventional procedures fail
Çağla Çiçek , Mustafa Özyildirim
, Mustafa Özyildirim , Alperen Kahraman
, Alperen Kahraman , Gaye Filinte
, Gaye Filinte
Department of Plastic, Aesthetic and Reconstructive Surgery, University of Health Sciences, Kartal Dr. Lutfi Kirdar City Hospital, Istanbul, Turkey
Address for correspondence: Çağla Çiçek, Department of Plastic, Aesthetic and Reconstructive Surgery, University of Health Sciences, Kartal Dr. Lutfi Kirdar City Hospital, D-100 South Yanyol, Cevizli Mevkii No:47, 34865 Kartal/Istanbul, Turkey, e-mail: caglamutkan2002@gmail.com
Received: 4.05.2023
Accepted: 10.06.2023
Publication: 7.07.2023
LECZENIE RAN 2023; 20 (2): 63–69
Table of contents:
Abstract
Introduction: Wounds that cannot be treated with conventional wound care procedures or those that do not become sufficiently smaller with 6 weeks of treatment are usually considered for reconstructive procedures. The present study reviews surgical procedures based on the reconstructive ladder used for the treatment of difficult wounds that contain cavities or are located on vital organs or tissues and do not heal with standard wound care. This review, which highlights that using conventional techniques in such wounds may be a waste of time and money, is intended to guide health professionals dealing with difficult wounds.
Material and methods: Between 2018 and 2023, 37 patients with full-thickness wounds due to various aetiologies were retrospectively investigated. The aetiologies, associated comorbidities, the timing, and the choice of surgical techniques were reviewed. The wounds that did not demonstrate a decrease in wound diameter with conventional wound care in 6 weeks were included in the study.
Results: The mean age of patients was 56.11 years (range 32–80), and the sex was predominantly male (75%). The number of surgeries were between 1 and 3 (mean 2). The length of hospital stay after surgery was 3–7 days (mean 4.2). Surgical wound infection (7), flap failure (3), and haematoma (2) were seen as complications.
Conclusions: Full-thickness wounds with deep cavities and wounds over vital structures usually do not respond to conventional wound care efficiently. A wound care specialist should be able to decide when to refer or perform surgery for the wound care patients. In wounds where wound closure is not possible with wound care alone, the patient should be delivered the most ideal method as soon as possible, taking into account surgical complications.
Key words: chronic wound, non-healing wound, reconstruction ladder, free flap, skin graft.
Introduction
A wound can be defined as a disruption of the normal anatomical relationships and integrity of tissues. Such a disruption triggers the wound healing process for the formation of new tissue. Wound healing follows a natural cellular process provided that the wound does not contain dead tissue or foreign bodies [1]. The wound healing process can be roughly divided into inflammation, proliferation, and remodeling phases [2]. Wound healing is a complex process involving all systems. A wound that does not heal in 4 to 6 weeks or does not regress by 20–40% despite 2 to 4 weeks of treatment can be defined as a chronic wound [3]. Surgery is a useful option in chronic wound management. Adequate surgery in chronic wounds aims to eliminate dead tissue [4]. In trying to heal wounds and prepare patients for repeat procedures, the primary goal is to determine the underlying aetiology and to correct etiologic causes where possible and eliminate comorbidities [5]. Universally accepted wound healing procedures may sometimes fail to achieve adequate wound healing despite correction of all comorbidities. This is particularly the case with wounds located on vital organs, cavity wounds, and full-thickness chronic tissue defects. Difficult wounds are those that do not heal with conservative treatment, do not heal with repeat procedures, and do not heal despite optimization of factors affecting wound healing. The present study presents some difficult cases followed and treated in our clinic and is intended to guide clinicians dealing with difficult wounds.
Material and methods
Between 2018 and 2023, 37 patients with full-thickness wounds of various aetiologies were retrospectively reviewed. The study was approved by the Ethics Committee of Kartal Dr. Lütfi Kırdar City Hospital and was conducted in accordance with the principles of the Declaration of Helsinki. The study included wounds that did not get smaller with 6 weeks of conventional wound care. Medical records were screened to retrieve patient data from the hospital registration system. A number of parameters were retrospectively analysed including age, sex, presence of comorbidities, length of postoperative hospital stay, wound size, complications, smoking status, location of the wound, surgical procedure performed, C-reactive protein levels at admission, and choice of surgical techniques. Complications were classified as minor or major and included wound dehiscence, hematoma, seroma, wound infection, and graft/flap loss [6]. Complications were considered major if they required surgical intervention and minor if they did not require surgical intervention.
Results
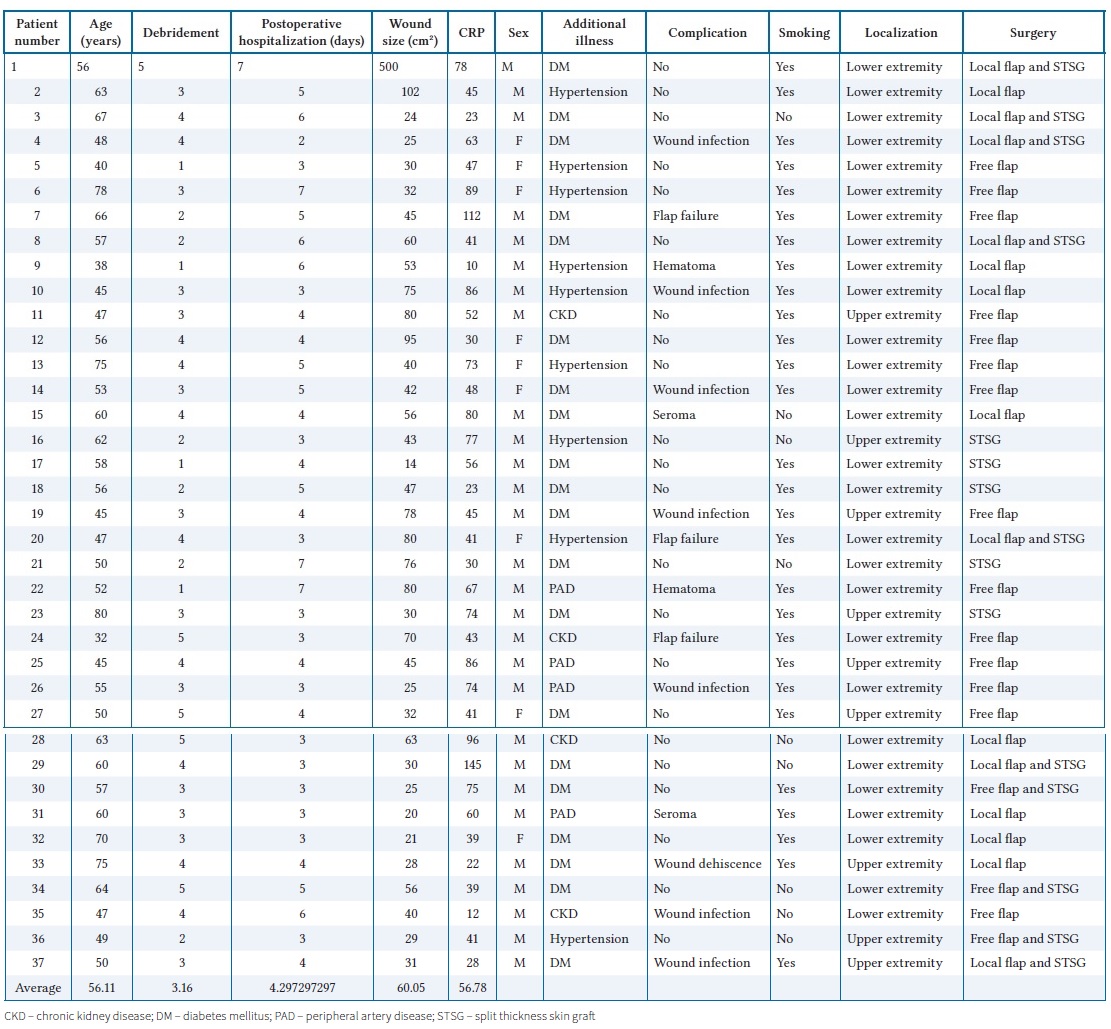
The study analysed 37 patients. The mean age of the patients was 56.11 years (32–80) and the majority were male (75%). Of the patients, 20 had diabetes mellitus, of whom 17 had type 2 diabetes mellitus and 3 had type 1 diabetes mellitus. Nine patients had hypertension. Four patients had chronic kidney disease and 4 patients had peripheral arterial disease. All patients received antibiotic therapy and nutritional support. The number of surgeries ranged from 1 to 3 (mean 2). All patients received debridement for three times on average (range: 1 to 5). The length of hospital stay after surgery was 3 to 7 days (mean: 4.2). Observed complications comprised surgical wound infection (7), flap failure (3), and haematoma (2). Three patients were scheduled for surgery due to flap failure. Complications requiring surgery were considered as major, while complications not requiring surgery were classified as minor. Of the patients, 28 were smokers. The wound was located on the lower extremities in 28 patients and on the upper extremities in nine patients. Of the patients, 18 underwent free flap reconstruction, 14 underwent local flap reconstruction, and 15 underwent graft reconstruction. Demographic and clinical characteristics of the patients are summarized in Table I.
Table I. Demographic data of patients
Case reports
Patient no. 1
A 56-year-old male patient presented to our outpatient clinic with a tissue defect in the right inguinal region. The patient’s medical history revealed a right below-knee amputation by the Orthopaedics and Traumatology Clinic about 3 months prior to presentation to our clinic; the patient had undergone hemipelvectomy for failure of the stump to heal after amputation. The patient had been treated with various wound care products and was then referred to our clinic because of non-closure of the wound. The patient had uncontrolled type 2 diabetes and had a history of smoking. Examination revealed a purulent, foul-smelling 20 × 25-cm2 cavity tissue defect on the amputation stump with an exposed acetabular joint. The patient was hospitalized in our clinic, and deep tissue cultures were obtained on admission. The CRP level was 78 on admission. Tissue culture revealed Acinetobacter baumannii growth, so the patient was started on meropenem therapy by the Department of Infectious Diseases. We then applied several sessions of debridement and 5 sessions of negative pressure wound therapy on the tissue defect, which prepared the wound for surgery (Fig. 1A), and then performed a rectus abdominis muscle flap based on the inferior epigastric artery and adapted it to the recipient site (Fig. 1B, C). The flap was covered with a partial-thickness skin graft. The patient had no complications in the early postoperative period and was discharged with recovery on day 7 of surgery (Fig. 1D, postoperative).
Patient no. 2
A 63-year-old male patient presented to our clinic with a tissue defect in the left inguinal region. The patient’s medical history revealed that he had type 2 diabetes mellitus and was a smoker. It was found that the tissue defect developed after debridement performed by an external orthopaedics and traumatology clinic for necrotizing fasciitis in the left inguinal region; during debridement, a pseudoaneurysm was detected in the left femoral artery. The cardiovascular surgery team performed a femoral artery bypass using a vascular graft (Fig. 2A); during follow-up, the patient developed a 7 × 15-cm2 tissue defect in this region with an exposed vascular graft. The patient was followed up using conventional wound care procedures in an external centre for 6 weeks and was referred to our clinic due to nonclosure of the wound. The patient was considered ineligible for negative-pressure wound therapy and repair with skin graft due to the risk of rupture and was thus scheduled for regional flap reconstruction. Wound culture obtained from the patient at admission revealed
E. coli growth. The CRP level at admission was 45. The patient received blood transfusion, ampicillin-sulbactam therapy, and repeat debridement procedures until the wound was prepared for surgery. Then, the wound was repaired using a random fasciocutaneous abdominal flap (Fig. 2B). Femoral neurovascular structures were covered, resulting in wound closure (Fig. 2C). The patient was followed up in the ward for 5 days and discharged with recovery.
Patient no. 3
A 67-year-old male patient presented to our outpatient clinic with tissue defect on the left foot with an exposed tendon (Fig. 3A). The patient had diabetes mellitus and rheumatoid arthritis. Medical history revealed that the patient presented to the Orthopaedics and Traumatology Clinic with a sprain in 2019 and was diagnosed with Achilles tendon rupture and underwent Achilles tendon repair in the Orthopaedics and Traumatology Department of our hospital. During follow-up, the patient had erythema and foul-smelling drainage at the wound site suggestive of wound infection. The tissue defect was 8 × 3 cm2 (Fig. 3A). The Achilles tendon was exposed in the tissue defect. Wound culture obtained from the tissue defect revealed Pseudomonas aeruginosa growth. The patient had a CRP level of 23 on admission. Upon recommendation from the Infectious Diseases Department, the patient was started on piperacillin and tazobactam therapy. The wound was prepared for surgery after 10 sessions of hyperbaric oxygen therapy, multiple sessions of debridement, and application of dermis-equivalent materials. The patient received antibiotic therapy and hydration therapy while waiting for surgery. Our clinic repaired the tissue defect using multiple grafts at different times. The tissue defect persisted during follow-up, upon which the patient was scheduled for free flap reconstruction. The patient then underwent radiographic imaging and was scheduled for repair of the defect using a left free radial forearm flap (Fig. 3B). Intraoperative fluorescein and ICG angiography showed that the free flap had a good blood supply in the recipient area (Fig. 3C). The defect was repaired using a free flap (Fig. 3D). The patient was followed up for 6 days in our clinic and was discharged with recovery.
Discussion
Chronic wounds are characterized by problems in every stage of healing. Wound healing is affected by many systemic and local risk factors, including age, sex, race, hypertension, obesity, diabetes mellitus, congestive heart failure, depression, history of smoking, and the presence of an inflammatory or autoimmune condition predisposing to chronic steroid use. It is inevitable that some wounds will be treated differently from conventional treatment techniques. In wounds that contain cavities, have exposed viable tissues, such as tendons, vessels, and nerves, are not granulated and do not get smaller despite 6 weeks of conventional treatment, flap or graft repair should be considered. Regardless of which option we use in the reconstruction step, patients should first be assessed using the TIME concept (tissue, infection, moisture balance, epithelial edge advancement). The TIME approach is a general wound management strategy developed for chronic wounds, which has been adapted based on physicians’ expertise [7]. The reconstructive pyramid is a tenet of plastic surgery in which soft tissue coverage techniques are arranged hierarchically, from minimally invasive procedures for small and superficial wounds to highly complex procedures for large, deep, and complicated soft tissue defects [8]. Treating physicians should gradually move up the reconstructive ladder from simple to more complex options but should bear in mind that some cases require starting on the highest rung. In plastic surgery, treatment of difficult wounds should be based on the reconstructive ladder, with treatment sometimes starting at the first rung and, at other times, at a higher rung by skipping certain steps. The wound care team should be able to decide at what stage reconstructive surgery should be used for wounds that do not close with normal wound care. The wound care team should be well trained on wound care techniques, able to perform conservative wound care, should know when wounds become suitable for surgical intervention, and in such cases, should refer patients to reconstructive surgeons without delay. There is no clear time frame for surgical interventions in tissue defects [9]. In the present study, the mean time to surgery was approximately 15 days (range: 5–47). Our clinic avoids intervening in chronic and complicated wounds too early, because premature intervention can further complicate the wound and may even result in limb loss. It also increases the costs. In the present study, 18 of the 37 patients underwent free flap reconstruction. In a study involving a free flap series of 506 patients with different aetiologies, Brady et al. reported that 50% of the patients had diabetes mellitus [10]. Z-Hye Lee et al. investigated the aetiology of wounds and reported that 15% of patients were smokers, 12% had coronary artery disease, and 12% had end-stage renal disease [11]. In our study, on the other hand, 54% of the patients had diabetes, 24% had hypertension, and 10% had peripheral arterial disease. Of the patients included in the present study, 75% were smokers. This suggests that smoking may cause cavity wounds that may require reconstructive surgery. Although wounds are classified as complicated when they do not respond to conservative treatment, the management of complicated wounds may need to make use of stromal vascular fraction, platelet-rich plasma, hyperbaric oxygen therapy, negative pressure wound therapy and specialized wound care products, because appropriate surgical procedure alone is not enough for wound closure. Hyperbaric oxygen therapy (HBOT) helps deliver oxygen support to the tissues in the wound and contributes to the healing process [12]. Our hospital has a dedicated unit for hyperbaric oxygen therapy, which was used in 9 cases that were difficult to manage; hyperbaric therapy was delivered preoperatively in 5 patients and postoperatively in 4 patients. The present study has a major limitation: it is a retrospective study and not a randomized controlled study. Management of complicated wounds warrants further studies. Wound management should use a multidisciplinary approach and should not be limited to a single technique. Finally, all health professionals dealing with wounds should be trained periodically and keep their knowledge on innovations up to date. To avoid wasting time and money in dealing with chronic wounds, health professionals in this field should be able to decide when to refer patients for wound care or surgery. Moreover, reconstructive surgeons dealing with closure of such wounds should be comfortable with moving up and down the reconstructive ladder depending on the patient’s clinical picture.
Conclusions
In conclusion, full-thickness wounds with deep cavities and wounds located over vital structures often fail to respond effectively to conventional wound care, and the management of these patients should be multidisciplinary and multifaceted.
Disclosure
The authors declare no conflict of interest.
References
- Zhou L, Tang J, Bai JJ, Ming Y. Wound care in elderly diabetic patients after coronary artery bypass grafting: Report of 3 cases. Asian J Surg 2022; 45: 759–760. DOI: 10.1016/j.asjsur.
2021.11.050. - Caldwell MD. Wound surgery. Surg Clin North Am 2010; 90: 1125–1132. DOI: 10.1016/j.suc.2010.09.001.
- Melikian R, O’Donnell TF Jr, Suarez L, Iafrati MD. Risk factors associated with the venous leg ulcer that fails to heal after 1 year of treatment. J Vasc Surg Venous Lymphat Disord 2019; 7: 98–105. DOI: 10.1016/j.jvsv.2018.07.014.
- Schultz GS, Sibbald RG, Falanga V, et al. Wound bed preparation: a systematic approach to wound management. Wound Repair Regen 2003; 11 Suppl 1: S1–S28. DOI: 10.1046/j.1524-475x.11.s2.1.x.
- Schubert S, Marzloff G, Ryder S, et al. Establishing a Comprehensive Wound Care Team and Program. Phys Med Rehabil Clin N Am 2022; 33: 805–810. DOI: 10.1016/j.pmr.2022.06.006.
- Perisanidis C, Herberger B, Papadogeorgakis N, et al. Complications after free flap Maxillofac Surg 2012; 50: 113–118. DOI: 10.1016/
j.bjoms.2011.01.013. - Strunck JL, Cutler B, Latour E, Seminario-Vidal L, Ortega-Loayza AG. Wound care dressings for pyoderma gangrenosum. J Am Acad Dermatol 2022; 86: 458–460. DOI: 10.1016/j.jaad.2021.09.053.
- Capobianco CM, Stapleton JJ, Zgonis T. Soft tissue reconstruction pyramid in the diabetic foot. Foot Ankle Spec 2010; 3: 241–248. DOI: 10.1177/1938640010375113.
- Lee ZH, Daar DA, Stranix JT, et al. Free-Flap Reconstruction for Diabetic Lower Extremity Limb Salvage. J Surg Res 2020; 248: 165–170. DOI: 10.1016/j.jss.2019.12.008.
- Brady JS, Govindan A, Crippen MM, et al. Impact of diabetes on free flap surgery of the head and neck: A NSQIP analysis. Microsurgery 2018; 38: 504–511. DOI: 10.1002/micr.30276.
- Wang KY, Lin YS, Chen LW, et al. Risk of Free Flap Failure in Head and Neck Reconstruction: Analysis of 21,548 Cases From A Nationwide Database. Ann Plast Surg. 2020; 84 (1S Suppl 1): S3–S6. DOI: 10.1097/SAP.0000000000002180.
- Kranke P, Bennett MH, Martyn-St James M, Schnabel A, Debus SE, Weibel S. Hyperbaric oxygen therapy for chronic wounds. Cochrane Database Syst Rev 2015; 2015 (6): CD004123. DOI: 10.1002/14651858.CD004123.pub4.
- Corbitt C, Skoracki RJ, Yu P, Hanasono MM. Free flap failure in head and neck reconstruction. Head Neck 2014; 36: 1440–1445. DOI: 10.1002/hed.23471.
- Yu J, Hong JP, Suh HP, et al. Prognostic Nutritional Index is a Predictor of Free Flap Failure in Extremity Reconstruction. Nutrients 2020; 12: 562. DOI: 10.3390/nu12020562.
- Han G, Ceilley R. Chronic Wound Healing: A Review of Current Management and Treatments. Adv Ther 2017; 34: 599–610. DOI: 10.1007/s12325-017-0478-y.

