Original paper | Praca oryginalna
Skin tears in nursing practice – preventive measures based on risk factor assessment
Rozdarcia skóry w praktyce pielęgniarskiej – podejmowanie działań profilaktycznych na podstawie oceny czynników ryzyka
Katarzyna Cierzniakowska![]() 1,2; Daria Borucka1, Elżbieta Kozłowska
1,2; Daria Borucka1, Elżbieta Kozłowska![]() 1, Beata Strzyżewska2, Aleksandra Popow
1, Beata Strzyżewska2, Aleksandra Popow![]() 1
1
1 Department of Interventional Nursing, Faculty of Health Sciences, Collegium Medicum in Bydgoszcz, Nicolaus Copernicus University in Torun, Polandd
2 Clinic of General and Minimally Invasive Surgery, Dr. J. Biziel University Hospital No. 2, Bydgoszcz, Poland
Address for correspondence: Katarzyna Cierzniakowska, Department of Interventional Nursing, Faculty of Health Sciences, Collegium Medicum in Bydgoszcz, Nicolaus Copernicus University in Torun, 1 Łukasiewicza St., 85-821 Bydgoszcz, Poland, e-mail: katarzyna.cierzniakowska@cm.umk.pl
Received: 17.11.2024 Accepted: 27.11.2024
Table of contents:
Abstract
Introduction: Skin tears (ST) are defined as traumatic wounds caused by mechanical forces (shearing, friction, and/or blunt trauma, including the removal of medical adhesives). They are most commonly observed in elderly individuals with chronic comorbidities, in critical condition, or at the end of life.
Aim of the study: To identify the best nursing and therapeutic practices undertaken by nurses to prevent ST based on risk factors identified in clinical research.
Material and methods: The study involved a review of the literature based on original research concerning traumatic skin injuries. The following databases were searched: Medline (EBSCO), Medline (PubMed), and Web of Science. The search criteria included the keywords: skin tear, risk factors, frequency, and prevalence.
Results: The analysis of research studies identified the following major risk factors for the occurrence of ST: advanced age and related changes in skin properties (loss of elasticity, dryness, and increased susceptibility to injuries), the presence of vascular changes (petechiae, senile purpura, hematomas), malnutrition, dependency on caregiver support, falls, and a history of previous skin tears. Reducing the occurrence of ST is achievable through highly qualified and experienced medical staff, comprehensive clinical assessments of patient risk, systematic skin monitoring and care, attention to the patient’s environment, and caregiver education.
Conclusions: Understanding and identifying the risk factors for ST are critical for effective management of these skin injuries and for improving the quality of healthcare. The implementation of preventive strategies and educational activities based on scientific evidence is essential for reducing the frequency and severity of ST in clinical practice.
Key words: skin tears, risk factors, incidence, prevention.
Streszczenie
Wprowadzenie: Rozdarcia skóry (skin tears – ST) są definiowane jako rany pourazowe spowodowane siłami mechanicznymi (siły ścinające, tarcie i/lub tępe uderzenie oraz usuwanie klejów medycznych). Najczęściej rozpoznawane są u osób w podeszłym wieku ze współistniejącymi schorzeniami przewlekłymi, w stanie krytycznym i u kresu życia.
Cel pracy: Wskazanie najlepszych praktyk pielęgnacyjno-terapeutycznych podejmowanych przez pielęgniarki w zapobieganiu ST na podstawie czynników ryzyka zidentyfikowanych w badaniach klinicznych.
Materiały i metody: W pracy dokonano przeglądu piśmiennictwa na podstawie prac oryginalnych dotyczących urazowego uszkodzenia skóry. Przeszukano bazy danych: Medline (EBSCO), Medline (PubMed) oraz Web of Science. Kryterium wyszukiwania były słowa kluczowe: rozdarcie naskórka, czynniki ryzyka, częstotliwość występowania, rozpowszechnianie.
Wyniki: Na podstawie analizowanych prac badawczych zidentyfikowano następujące główne czynniki ryzyka występowania ST: zaawansowany wiek oraz związane z nim zmiany właściwości skóry (utrata elastyczności skóry, suchość i zwiększona podatność na urazy), obecność zmian naczyniowych (wybroczyny, plamica starcza, krwiaki), niedożywienie, uzależnienie od opieki świadczonej przez innych, upadki oraz przebyte ST w przeszłości. Redukcja występowania ST u chorych jest możliwa pod warunkiem wysokich kwalifikacji i doświadczenia kadry medycznej, całościowej oceny stanu klinicznego chorego pod kątem ryzyka, systematycznego monitorowania stanu skóry i jej pielęgnacji, dbałości o środowisko chorego i edukację opiekunów.
Wnioski: Znajomość i identyfikacja czynników ryzyka ST są kluczowe dla skutecznego zarządzania tym rodzajem urazów skóry oraz poprawy jakości opieki zdrowotnej. Wdrożenie do praktyki klinicznej strategii prewencyjnych i działań edukacyjnych opracowanych w oparciu o dowody naukowe, ma fundamentalne znaczenie w redukcji częstości i nasilenia ST.
Słowa kluczowe: rozdarcie skóry, czynniki ryzyka, częstość występowania, profilaktyka.
Introduction
In 2011, experts from the International Skin Tear Advisory Panel (ISTAP) standardized the terminology by defining skin tears (ST) as wounds caused by shear, friction, and/or blunt forces that lead to the separation of skin layers. Skin tears can involve either partial-thickness injuries (separation of the epidermis from the dermis) or full-thickness injuries (separation of the epidermis and dermis from underlying structures) [1, 2]. The definition was later refined to specify that ST are traumatic wounds caused by mechanical forces, including the removal of medical adhesives. Their classification varies based on depth (not exceeding the subcutaneous layer) and includes three categories:
- type 1: No skin loss,
- type 2: Partial loss of damaged skin/flap,
- type 3: Complete loss of damaged skin/flap.
In the context of ST, a “flap” is defined as a portion of skin (epidermis/dermis) that is unintentionally separated (partially or completely) from its original position due to shearing, friction, and/or blunt force. This term should not be confused with tissue that is intentionally separated for therapeutic purposes, such as for surgical skin grafting [3].
Skin tears can occur at any age. They are most commonly diagnosed in elderly individuals with chronic comorbidities, in critical condition, or at the end of life. However, they can also occur in children and premature infants. The injuries are most frequently located on the extremities [4–6].
Risk factors
Skin tears represent one of the most common skin-related issues among elderly individuals. They are often not properly recognized or reported and are frequently misdiagnosed, for example, as lacerations [1, 7]. Skin tears negatively affect the quality of life of older adults by causing pain, suffering, and infection, prolonging hospital stays, increasing healthcare costs, and complicating patient care. For these reasons, early identification of risk factors for ST is crucial [8].
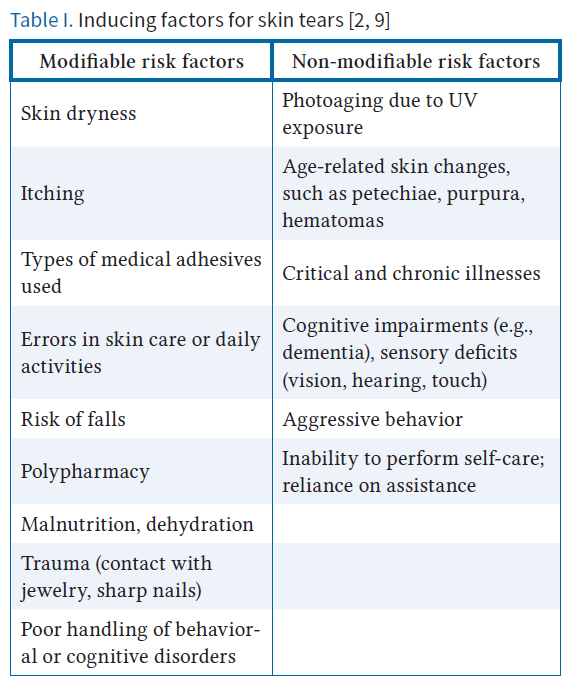
A comprehensive risk assessment for ST involves evaluating the patient’s overall health, mobility, and skin condition. Various factors can contribute to the occurrence of ST, as summarized in Table I.
The role of nurses in managing skin tears
A comprehensive risk assessment includes evaluating the patient’s general health (chronic illnesses, polypharmacy, cognitive and sensory functions, and nutritional status), mobility (history of falls, restricted mobility, reliance on others for daily activities, and mechanical injuries), and skin condition (including skin sensitivity to trauma and previous occurrences of ST). An essential aspect of managing ST is the use of established classification systems for identifying and documenting wounds and making therapeutic decisions based on wound management protocols [10, 11].
In the context of preventing and treating skin injuries, particularly among elderly patients, teamwork and a holistic approach to care are crucial. Nurses specializing in wound care play a key role in educating patients and their caregivers about maintaining healthy skin and implementing preventive methods. These efforts contribute to improving skin properties, preserving its integrity, and reducing the risk of new injuries [12–14].
Accurate documentation, which includes noting risk factors and providing detailed descriptions of wounds, is a priority for effective wound assessment. Nurses regularly evaluate all skin injuries, including ST, using specialized tools recommended by ISTAP. The documentation includes measurements of each ST, their location, the quantity and color of exudate, and the type of dressing applied. This allows for precise monitoring and appropriate therapy planning [2].
Aim of the study
The aim of the study was to identify the best nursing and therapeutic practices undertaken by nurses to prevent ST based on the risk factors identified in clinical research.
Material and methods
The study involved a literature review of original papers concerning traumatic skin damage. The databases searched included Medline (EBSCO), Medline (PubMed), and Web of Science. The search criteria included the keywords: “skin tear,” “risk factors,” “incidence,” and “prevalence.” Full-text articles published in the past ten years that contained data on the incidence and risk factors for ST were analyzed. Abstracts and conference reports were excluded from the analysis.
Research results
The analyzed studies focused on assessing the prevalence of ST, identifying risk factors, and examining the properties of skin affected by this condition. All the studies were conducted among adult patients. The prevalence of ST varied significantly, ranging from 3% in a population of 795 nursing home residents (mean age 85 years) [15] to 41% in a group of 173 nursing home residents in another country (mean age 87.6 years, 6-month observation period) [7].
A multivariate analysis conducted in an Australian study confirmed the significant impact of individual characteristics and adverse events on the occurrence of ST. These included gender (men were three times more likely than women to experience ST), prior ST within the past 12 months, falls in the preceding 3 months, and additional factors such as signs of elastosis and senile purpura [7]. Another Australian study examined the characteristics associated with ST among hospitalized patients. The data analyzed included 151 hospitalized individuals who experienced ST up to 5 days before hospital admission or during their stay, compared with 302 patients without skin injuries. Several critical factors contributing to skin tears were identified, including advanced age, senile purpura, petechiae, hematomas, fragile and dry skin, previously healed ST, cognitive impairment, and chronic diseases such as chronic obstructive pulmonary disease, malignant lymphoma, myocardial infarction, diabetes complications, and vascular diseases. Other contributing factors included skin edema, contractures, and the inability to change positions independently. Multivariate analysis demonstrated that the risk of ST increased 2 to 6 times in patients with petechiae, previously healed ST, senile purpura, edema, hematomas, and those unable to change positions independently [16].
The multivariate analysis indicates that advanced patient age and related changes in skin properties, such as reduced elasticity, dryness, and increased vulnerability to injuries, were the dominant factors contributing to the occurrence of ST [17–20]. Additionally, vascular skin changes such as petechiae, senile purpura, hematomas, and edema were identified as significant contributors [7, 15, 17, 18, 21, 22], along with a history of previous ST [7, 15, 16, 19, 22, 23]. Studies conducted in Japan across various long-term care facilities reported the prevalence of ST ranging from 3.8% to 13.5% of patients. In this population, repeated risk factors included skin features such as senile purpura, bruises, hematomas, previously healed ST, scars, dry skin, and contractures. These findings were further compounded by exposure to shearing and friction forces during repositioning, as well as the use of corticosteroids and anticoagulants [20, 23, 24]. Additional independent predictors of ST included dementia [18], malnutrition, low body mass index (BMI), and reduced albumin levels [18, 21]. Other significant risk factors identified were falls [7, 19], the use of adhesives or dressings [15], and the frequently highlighted loss of mobility, which resulted in dependency on caregivers. This dependency, when coupled with a lack of caregiver knowledge and skills, exposed patients to an increased risk of skin integrity loss [15, 16, 18, 20].
These risk factors are crucial for the effective identification of patients at risk of ST and the implementation of appropriate preventive strategies and care management. The role of nurses in monitoring, educating, and implementing suitable interventions is pivotal for minimizing risks and ensuring high-quality care.
Discussion of research results
The selected studies focused on evaluating the prevalence of ST and identifying the primary risk factors associated with these types of skin injuries to propose the best practices for preventing their occurrence and mitigating their consequences when they do arise.
Considering the prevalence of ST in various residential care facilities and home care settings, it is often challenging to compare the reported values across studies. These values vary significantly, even among facilities with similar profiles. For instance, Hawk et al. reported that in six facilities in western Pennsylvania, the prevalence of ST ranged from 3% to 16% [25]. Other researchers have described the prevalence of skin injuries using incidence rates expressed as cases per 1,000 patient-days [26]. The considerable variability in published data regarding the prevalence of ST may partly be attributed to suboptimal recognition and reporting practices among healthcare workers [27]. Consequently, the actual prevalence of ST is likely higher than the reported figures [25].
Nevertheless, the prevalence data presented by researchers deserve deeper analysis and highlight the need to implement effective prevention and management strategies for ST into nursing practice. Establishing evidence-based protocols for identifying, reporting, and addressing ST can significantly improve outcomes and reduce the burden of these injuries on patients and healthcare systems.
Prevention of skin tears
High qualifications and clinical experience among nurses are critical for preventing and/or reducing the incidence of ST [28, 29]. Identifying numerous risk factors for ST, especially modifiable internal and external factors, enables the development and implementation of individualized care plans for patients.
The prevention strategy for ST should be based on several pillars:
-
Evaluating the occurrence and progression of changes resulting from the aging process and multimorbidity is crucial.
Soh et al. observed that individuals with dementia might be more susceptible to injuries due to limited awareness and difficulties in cooperating during care. The high risk of falls associated with dementia, potential self-harm, and impaired awareness of hazards further increase the likelihood of skin injuries [18]. Sensory deficits, such as impaired touch, vision, and hearing, also represent significant risk factors [21]. In this context, care should focus on ensuring a safe environment for the patient. Studies confirm that falls are a significant, long-term risk factor associated with skin injuries [7, 19, 18, 21]. Therefore, providing a safe environment and adequate protective measures is essential for preventing potential skin injuries in patients.
Patients with more than one chronic condition tend to exhibit a more complex propensity for developing ST [21]. Furthermore, studies have identified a significant association between the use of corticosteroids and anticoagulants and the occurrence of skin injuries. The use of steroids can inhibit collagen synthesis, reduce the tensile strength of the skin, and impair the viability of tenocytes, thereby increasing susceptibility to skin injuries. Anticoagulants, on the other hand, may lead to soft tissue damage even with minor trauma and negatively affect wound healing processes by modifying blood flow and coagulation mechanisms [15, 20, 21].
Nurses play a critical role not only in informing patients about the side effects and risks associated with the use of steroids or anticoagulants but also in continuously monitoring the condition of the skin. Through regular assessments, they can quickly identify potential skin injuries and take appropriate preventive and therapeutic actions. Their involvement in monitoring skin conditions is essential for ensuring proper care and minimizing the risk of complications in patients using these medications [2].
Particular caution should be exercised when caring for patients with extreme BMI values (<20 or > 30 kg m²). Lower BMI may lead to reduced skin thickness, which increases vulnerability to injuries. Researchers have demonstrated a statistically significant relationship between skin injuries, BMI, albumin levels, and malnutrition. Albumin deficiency has been identified as an independent risk factor for compromised skin integrity. It may contribute to the formation of skin injuries through its association with nutritional status and as a negative acute-phase reactive protein, influencing the mechanism of edema [18, 21]. Regular assessment and optimal nutritional support tailored to the patient’s needs are critical not only for preventing but also for treating ST.
Standardized health assessment tools are valuable in evaluating the patient’s condition. Although the Braden Scale is commonly used in clinical practice for predicting pressure ulcers, it can also effectively serve as a prognostic tool for ST. The scale assesses several key factors: sensory perception, skin moisture, activity, mobility, nutritional status, and the impact of friction and pressure forces. Using this scale, at-risk individuals can be identified, and appropriate preventive measures can be implemented, such as regular repositioning, the use of specialized cushions and mattresses, and skin care routines. The Braden Scale also enables tracking the effectiveness of preventive measures and adapting care plans to ensure the health and integrity of the patient’s skin [23].
-
Maintaining physical activity
Preventive measures in this area include encouraging patients to remain physically active, provided there are no significant functional deficits. Attention should be given to selecting appropriate assistive devices, such as walkers or wheelchairs, and securing the bed with railings during sleep. In patient care, it is essential to provide comfortable footwear, ensure proper lighting in the room, and remove rugs to minimize fall risks [2].
Some nursing interventions and actions increase the risk of ST in patients [30]. In ST prevention programs, special attention should be given to patients who are entirely dependent on others for care. These individuals often experience ST during routine activities such as dressing, bathing, repositioning, and transferring. Frequent manipulation to change positions can exacerbate the effects of shear forces, friction, or other skin injuries resulting from maneuvers performed during patient care.
Skills in positioning and transferring patients should include techniques that reduce pressure on the skin, ensure a safe environment, and use specialized devices and equipment, such as anti-pressure mattresses, hoists, positioning aids, and glide sheets [15, 16, 18, 20, 21].
-
Skin care
Research on the structural and mechanical properties of the skin in individuals with ST has shown that progressive changes result from the fundamental effects of chronological aging as well as environmental and lifestyle influences [31]. With age, the skin gradually becomes less hydrated and thinner. It exhibits water loss in the epidermal layer, reduced elasticity, and a decreased ability to return to its original shape. These changes are associated with the degradation of collagen and elastin structures, which increases susceptibility to damage and weakens the skin’s healing mechanisms. Photoaging, resulting from UV radiation exposure, also contributes to the more frequent occurrence of skin injuries. The effects of photoaging include elastosis, characterized by thickened, scaly, dry, and stiff skin texture, particularly visible in areas exposed to UV radiation [7, 15, 17, 20, 21].
Among vascular skin changes that increase the risk of ST are petechiae (Figure 1), senile purpura, and hematomas. These are primarily caused by vascular fragility, but coagulation disorders and anticoagulant use also contribute to their development. Although hematomas have not always been recognized as a risk factor, they can increase skin tension, which can also lead to tearing (Figure 2) [7, 16, 19, 21, 24]. Edema negatively affects the epidermal barrier, reducing its resistance to external forces, which also increases the susceptibility to ST [16].
Regular assessment of skin condition enables the early detection of risks and allows for a swift and effective preventive response. The foundation of skin care includes maintaining hygiene (using non-rinse cleansers, drying the skin with gentle materials, moisturizing and lubricating regularly, and immediately cleaning contamination caused by urinary and/or fecal incontinence), protecting extremities by wearing clothing with sleeves and long pants, keeping nails trimmed short, and avoiding sharp objects such as jewelry [2, 32, 33, 34].
The use of adhesives/dressings on the skin can increase the risk of ST by as much as 7.05 times due to the external force required for their removal. The type of medical adhesive used also plays a significant role [15].
-
Education of patients and their caregivers
Some studies suggest that the prevalence of ST in home care settings is higher than in institutional care. To prevent ST, systematic education should be conducted in the patient’s environment. Engaging the patient and involving their caregivers in the care process grants them autonomy and enables them to take control of their health [35].
Accordingly, the tasks of nurses, physiotherapists, and medical caregivers include collaboration with the patient and their caregivers. This collaboration involves providing instructions, conducting workshops and training sessions on skin care, repositioning techniques, fall prevention, and informing caregivers of older adults about potential risks associated with skin injuries. Professionalism and care expressed through emotional support for patients at risk of ST can significantly improve their quality of life.
Conclusions
Understanding and identifying the risk factors for ST are crucial for effectively managing this type of skin injury and improving the quality of healthcare. Implementing evidence-based preventive strategies and educational interventions in clinical practice is fundamental for reducing the frequency and severity of ST.
Disclosures
The authors declare no conflict of interest.
This research received no external funding.
Approval of the Bioethics Committee was not required.
References
- Le Blanc K, Baranoski S. Skin tear consensus panel members. Skin tears: state of the science: consensus statements for the prevention, prediction, assessment, and treatment of skin tears©. Adv Skin Wound Care 2011; 24 (9 Suppl): 2–15.
- Campbell KE, Baronoski S, Gloeckner M, et al. Skin tears: Prediction, prevention, assessment and management. Nurse Prescribing 2018; 16: 600–607.
- Van Tiggelen H, LeBlanc K, Campbell K, et al. Standardizing the classification of skin tears: validity and reliability testing of the International Skin Tear Advisory Panel Classification System in 44 countries. Br J Dermatol 2020; 183: 146–154. DOI: 10.1111/bjd.18604.
- LeBlanc K, Campbell KE, Wood E, Beeckman D. Best Practice Recommendations for Prevention and Management of Skin Tears in Aged Skin: An Overview. J Wound Ostomy Continence Nurs 2018; 45: 540–542. DOI: 10.1097/WON.0000000000000481.
- Szymańska P, Bazaliński D, Szewczyk M. Skin tears in nursing practice – literature review versus own experience. Pielęg Chir Angiol 2021; 15: 155–162.
- Jani P, Mishra U, Buchmayer J, et al. Global variation in skin injures and skincare practices in extremely preterm infants. World J Pediatr 2023; 19: 139–157. DOI: 10.1007/s12519-022-00625-2.
- Rayner R, Carville K, Leslie G, Dhaliwal SS. A risk model for the prediction of skin tears in aged care residents: a prospective cohort study. Int Wound J 2019; 16: 52–63.
- Chen L, Zheng N, Jiang H, et al. Risk factors of skin tear in older persons: a protocol for systematic review and meta-analysis. BMJ Open 2024; 14: e080106. DOI: 10.1136/bmjopen-2023-080106.
- Le Blanc K, Baranoski S, Christensen D, et al. International Skin Tear Advisory Panel: a tool kit to aid in the prevention, assessment, and treatment of skin tears using a simplified classification system. Adv Skin Wound Care 2013; 26: 459–476. DOI: 10.1097/01.ASW.0000434056.04071.68.
- Benbow M. Assessment, prevention and management of skin tears. Nurs Older People 2017; 29: 31-39. DOI: 10.7748/nop.2017.e904.
- Miles SJ, Fulbrook P, Williams DM. Skin tear prevalence in an Australian acute care hospital: A 10-year analysis. Int Wound J 2022; 19: 1418–1427. DOI: 10.1111/iwj.13735.
- Bazaliński D, Szymańska P, Wójcik A. Traumatic partial-thickness skin injuries in clinical practice – a study of four cases. Leczenie Ran 2021; 162–170.
- Mitchell A. Skin assessment in adults. Br J Nurs 2022; 31: 274–278.
- Holloway S, Prentice J, Samuriwo R. Preventing, assessing and treating skin tears. Nurs Stand. 2023; 38: 37–45. DOI: 10.7748/ns.2023.e12127.
- Van Tiggelen H, Van Damme N, Theys S, et al. The prevalence and associated factors of skin tears in Belgian nursing homes: A cross-sectional observational study. J Tissue Viability 2019; 28: 100–106. DOI: 10.1016/j.jtv.2019.01.003.
- Lewin GF, Newall N, Alan JJ, et al. Identification of risk factors associated with the development of skin tears in hospitalised older persons: a case-control study. Int Wound J 2016; 13: 1246-1251. DOI: 10.1111/iwj.12490.
- Yuceler Kacmaz H, Kahraman H, Cinar SL, Ozkan F. Skin properties associated with skin tears in older adults: A case-control study. J Tissue Viability 2023; 32: 585–589. DOI: 10.1016/j.jtv.2023.09.004.
- Soh Z, Wang W, Png GK, Hassan N, Wu VX. Risk of skin tears and its predictors among hospitalized older adults in Singapore. Int J Nurs Pract 2019; 25: e12790. DOI: 10.1111/ijn.12790.
- Bermark S, Wahlers B, Gerber AL, et al. Prevalence of skin tears in the extremities in inpatients at a hospital in Denmark. Int Wound J 2018; 15: 212–217.
- Koyano Y, Nakagami G, Iizaka S, et al. Exploring the prevalence of skin tears and skin properties related to skin tears in elderly patients at a long-term medical facility in Japan. Int Wound J 2016; 13: 189–197. DOI: 10.1111/iwj.12251.
- Yüceler Kaçmaz H, Karadağ A, et al. The prevalence and factors associated with skin tears in hospitalized older adults: A point prevalence study. J Tissue Viability 2022; 31: 387–394. DOI: 10.1016/j.jtv.2022.06.001.
- Skiveren J, Wahlers B, Bermark S. Prevalence of skin tears in the extremities among elderly residents at a nursing home in Denmark. J Wound Care 2017; 26 (Suppl. 2): S32–S36.
- Sanada H, Nakagami G, Koyano Y, et al. Incidence of skin tears in the extremities among elderly patients at a long-term medical facility in Japan: A prospective cohort study. Geriatr Gerontol Int 2015; 15: 1058–1063. DOI: 10.1111/ggi.12405.
- Minematsu T, Dai M, Tamai N, et al. Risk scoring tool for forearm skin tears in Japanese older adults: A prospective cohort study. J Tissue Viability 2021; 30: 155–160. DOI: 10.1016/j.jtv.2021.02.010.
- Hawk J, Shannon M. Prevalence of Skin Tears in Elderly Patients: A Retrospective Chart Review of Incidence Reports in 6 Long-term Care Facilities. Ostomy Wound Manage 2018; 64: 30–36.
- Koyano Y, Nakagami G, Iizaka S, et al. Skin property can predict the development of skin tears among elderly patients: a prospective cohort study. Int Wound J 2017; 14: 691–697. DOI: 10.1111/iwj.12675.
- Blackburn J, Ousey K. Preventing and recognising skin tears using a standardised approach. Nurs Stand 2024; 39: 45–49. DOI: 10.7748/ns.2023.e12066.
- Jiang Q, He H, Jing K, et al. Knowledge status of skin tear prevention and its demographic and occupational influencing factors: A National cross-sectional survey among nurses. J Adv Nurs 2024; 00: 1–11. DOI: 10.1111/jan.16353.
- Kaçmaz HY, Karadağ A, Çakar V, Ödek Ö. Determination of Nurses’ Knowledge Levels on Skin Tears: A Cross-sectional Study. Adv Skin Wound Care 2023; 36: 267–274. DOI: 10.1097/01.ASW.0000922700.12014.e7.
- Cilluffo S, Bassola B, Beeckman D, Lusignani M. Risk of skin tears associated with nursing interventions: A systematic review. J Tissue Viability 2023; 32: 120–129. DOI: 10.1016/j.jtv.2022.11.006.
- Rayner RL, Carville KJ, Leslie GD, Dhaliwal SS. Clinical purpura and elastosis and their correlation with skin tears in an aged population. Arch Dermatol Res 2019; 311: 231–247. DOI: 10.1007/s00403-019-01899-9.
- Carville K, Leslie G, Osseiran-Moisson R, et al. The effectiveness of a twice-daily skin-moisturising regimen for reducing the incidence of skin tears. Int Wound J 2014; 11: 446–453. DOI: 10.1111/iwj.12326.
- Fastner A, Hauss A, Kottner J. Skin assessments and interventions for maintaining skin integrity in nursing practice: An umbrella review. Int J Nurs Stud 2023; 143: 104495. DOI: 10.1016/j.ijnurstu.2023.104495.
- Vuorinen M, Ram F. Effectiveness of moisturiser for the prevention of skin tears in older adults residing in long-term care facilities: a clinical review. Br J Community Nurs 2023; 28 (Suppl. 9): S14–S18. DOI: 10.12968/bjcn.2023.28.Sup9.S14.
- Beechey R, Priest L, Peters M, Moloney C. An evidence-based approach to the prevention and initial management of skin tears within the aged community setting: a best practice implementation project. JBI Database System Rev Implement Rep 2015; 13: 421–443. DOI: 10.11124/jbisrir-2015-2073.

